Dialysis Access Education
What is an arteriovenous fistula?
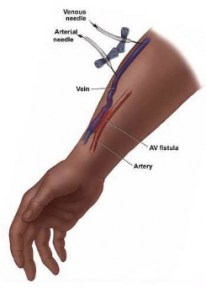
A surgeon creates an AV fistula by connecting an artery directly to a vein, frequently in the forearm. Connecting the artery to the vein causes more blood to flow into the vein. As a result, the vein grows larger and stronger, making repeated needle insertions for hemodialysis treatments easier.
An AV fistula requires advance planning because a fistula takes a while after surgery to develop—in rare cases, as long as 2-4 months – but a properly formed fistula is less likely than other kinds of vascular access to form clots or become infected. Also, properly formed fistulas tend to last many years—longer than any other kind of vascular access.
What is an arteriovenous graft?
If you have small veins that won’t develop properly into a fistula, you can get a vascular access that connects an artery to a vein using a synthetic tube, or graft, implanted under the skin in your arm. The graft becomes an artificial vein that can be used repeatedly for needle placement and blood access during hemodialysis. A graft doesn’t need to develop as a fistula does, so it can be used sooner after placement, often within 2 or 3 weeks.
Compared with properly formed fistulas, grafts tend to have more problems with clotting and infection and need replacement sooner. However, a well-cared-for graft can last several years.
What is a venous catheter for temporary access?
If your kidney disease has progressed quickly, you may not have time to get permanent vascular access before you start hemodialysis treatments. You may need to use a venous catheter as a temporary access.
A catheter is a tube inserted into a vein in your neck, chest, or leg near the groin. It has two chambers to allow a two-way flow of blood. Once a catheter is placed, needle insertion is not necessary.
Catheters are not ideal for permanent access. They can clog, become infected, and cause narrowing of the veins in which they are placed. But if you need to start hemodialysis immediately, a catheter will work for several weeks or months while your permanent access develops.
Catheters that will be needed for more than about 3 weeks are designed to be tunneled under the skin to increase comfort and reduce complications. Even tunneled catheters, however, are prone to infection.
PVG Provides Solutions for Better Dialysis Care
Learn more about dialysis access creation and management by clicking on the links below:
Dialysis Access Options Dialysis Access Management Vascular Access Management ProgramIf you would like to schedule an appointment at Preferred Vascular Group to have a consult with a Board-Certified physician or would like to have one of our highly trained care providers reach out to you, please click on a button below: